Glaucoma
Early detection of glaucoma including Retinal Nerve Fibre Layer Analysis (GDX) and computerized automated visual field testing. Various treatment modalities for glaucoma including laser (YAG laser iridotomy, Selective Laser Trabeculoplasty) & microsurgery (Trabeculectomy & Drainage Valve surgery)
The Glaucoma Service at Saraswati Nethralaya
Sight is our most precious sense enabling us to enjoy the world around us. One of the leading causes of blindness is glaucoma. Unlike cataract, blindness due to glaucoma is permanent. While there are no known ways of preventing glaucoma, blindness or significant vision loss from glaucoma can be prevented if the disease is recognized in the early stages. At Saraswati Nethralaya, we have a dedicated team of eye specialists committed to provide you with the best possible care to protect your vision.
What is Glaucoma?
Glaucoma, otherwise known as Kala Motia is an eye disease in which there is an increase in pressure inside the eye. Just as some people have high blood pressure, in the same way a glaucoma patient has high eye pressure.
If the eye pressure remains high for a long time it damages the optic nerve which carries the light sense from the eye to the brain. This damage to the nerve is irreversible and leads to permanent and incurable blindness. That is why glaucoma is a dangerous disease of the eye and has been labeled as 'lurking thief of vision'. Glaucoma is the second leading cause of blindness in the world with 70 to 105 million people affected worldwide (WHO).
Why is it important to know about glaucoma?
Damage due to glaucoma is preventable, not curable. It is therefore necessary that the disease should be detected and treated at its earliest stage to prevent blindness.
How does a person come to know that he/she is suffering from glaucoma?
Glaucoma is usually asymptomatic or is associated with very mild symptoms which the patient often tends to ignore. Some of the early symptoms include:
Frequent change of reading glasses.
Mild eye ache or headache towards the evening after a day's work.
Seeing rainbow colored haloes of light around a bulb associated with slight decrease in vision.
Inability to adjust one's vision on entering a dark room. Difficulty in focusing on close work.
In advanced cases, there is a loss of side vision, while the central vision remains good. The patient becomes more prone to accidents as he/she is unable to see vehicles coming from the sides.
It is to be remembered, that cataract (Safed Motia) also starts developing at the same age as glaucoma. Many people may think that they are losing vision due to cataract whereas it may actually be due to glaucoma, which is a much more dangerous disease.
It is therefore advisable to undergo a routine examination around the age of 40 years to screen for glaucoma.

Which age does glaucoma affect?
Although glaucoma is most common above the age of 40 years, it may affect any age group. A special type of glaucoma called Congenital Glaucoma may affect even a newborn or a child. Any eye that appears bigger than normal in a child should be shown to an eye specialist.
Who all are at high risk of developing glaucoma?
Presence of glaucoma in other family members
Increasing age above 40 years
Thyroid disease o Patients who are on long term steroid therapy for other diseases such as asthma, arthritis etc.
Previous eye injury or surgery o Hypermetropia (farsightedness)
Damage due to glaucoma may be more severe in those patients who have associated diabetes, widely fluctuating blood pressure and myopia.
What are the types of glaucoma in adults?
There are three main varieties of glaucoma in adults which concern us:-
Chronic Glaucoma or Open-angle Glaucoma
Acute Glaucoma or Closed-angle Glaucoma
Secondary glaucoma, which develops due to systemic diseases like prolonged diabetes, complicated high blood pressure, thyroid disease, bleeding disorders etc. It may also occur as a complication of associated eye disorders such as vascular blocks, bleeding inside the eye, uveitis, swollen lens, blunt injury to the eye, etc.
What is the difference between Open-angle and Closed-angle glaucoma?
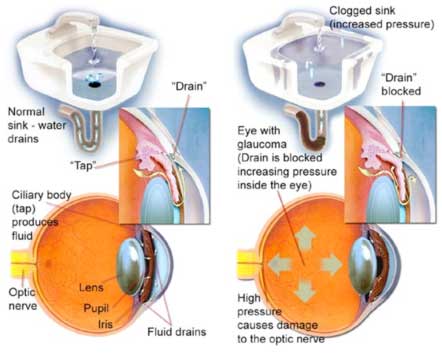
Let us explain with the simple example of a kitchen sink at your home. There is a tap through which water comes and there is a drain through which water, after cleaning utensils, is drained off. If the drain is blocked, water accumulates in the sink. Similarly, in your eye there is an area which produces a clear fluid which circulates inside the eye and provides oxygen and nourishment to the vital parts. Likewise, there is a small drainage channel through which all the waste products from inside the eye are drained. In glaucoma this passage or the drainage channel is blocked, either at its entrance or beyond. When the block is at the entrance it is called Closed Angle Glaucoma. When the blockage is not at the entrance, but beyond, somewhere inside, we call it Open Angle Glaucoma. The blockage results in more fluid accumulating inside the eye than can be drained out. This leads to a buildup of high pressure inside the eye.
How is glaucoma detected or diagnosed?
Vision testing
Since glaucoma more often affects the side vision, the central vision may be retained till a very advanced stage. It is important to remember that a good central (straight ahead)vision test may mislead a glaucoma patient about theseverity of glaucoma and the extent of damage to the optic nerve.
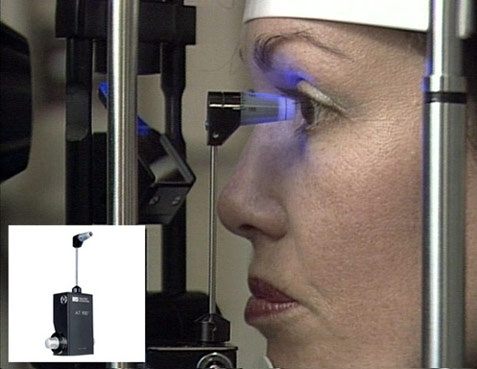
Measurement of eye pressure
This is done by tonometry (non-contact/applanation). This helps your doctor to determine how high your pressure is and how well the medicine is controlling it.
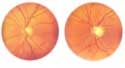
Evaluation of optic nerve damage
By ophthalmoscopy and optic nerve photography.
Evaluation of drainage channels
A special magnifying contact lens is used on your eye to help your doctor determine why the fluid is not draining properly. This examination is called gonioscopy.
Visual field examination
This test detects defects in your central and peripheral field of vision.
GDxVCC Retinal Nerve Fiber Layer Analyzer / HRT / OCT
These special tests measure the thickness of the nerve fibre layer and helps your doctor detect glaucoma at a very early stage.
How often should one get an eye check up?
After the age of 40 years, one should get an eye check up for glaucoma every 3 to 4 years even if there are no symptoms.
If a family member has glaucoma, if you have diabetes, if you are on long term systemic steroids for some other disease, or if you have suffered a blunt eye injury in the past, you must get your eyes checked every 1 to 2 years.
How is glaucoma treated?
As damage to nerve caused by glaucoma cannot be reversed, the aim of the treatment is to prevent or reduce further damage to the optic nerve. The first step to do that is to lower the eye pressure. The three modalities of treatment are:-
Medical (Eye drops and tablets) Laser treatment Surgery
Medical treatment:
Your doctor will prescribe you certain medication (Eye drops and tablets) so as to lower your eye pressure. R21; You must use the medicines regularly as directed by your ophthalmologist.
You should not stop medicines even if you do not have symptoms.
A regular follow up, as advised by your doctor, is mandatory.
Laser treatment:
If glaucoma is not controlled with the help of medicines, if the side effects of the medicines are not well tolerated and the patient is non compliant, or cannot afford the cost of the medicines, the second option is LASER TREATMENT. There are various types of lasers that are used in the treatment of glaucoma.
YAG Laser Peripheral Iridotomy
A small opening is made in the iris so that the stagnant fluid finds a way to the anterior chamber, the front portion of the eye, and subsequently drained off. This is an OPD procedure, done under local anesthetic drops and takes only a few minutes to be completed. After the laser, you can wash your eye with water and can lead a normal life.

Selective Laser Trabeculoplasty (SLT)
This is a new type of laser, which does not cause any thermal burn in the eye and may be called COLD LASERR. It stimulates the autoimmune system of the eye to clear the block in the drainage area without damaging the surrounding delicate tissues. SLT is a painless OPD procedure, which takes a few minutes to be completed. One can resume normal activities immediately after the laser. If necessary it can be safely repeated without damaging the eye.
Argon Laser Trabeculoplasty
When applied at the drainage area, the laser causes small burns, which contract to open up the block.
Diode Laser Cycloablation
In this the laser is applied on the area, which produces fluid in the eye. It can be used if the IOP is too high and is intractable.
Your treating doctor will decide which laser is suitable for you.
Operative procedures (Glaucoma Filtering Microsurgery )
Operation for glaucoma is the only option left for patients in whom the eye pressure is not controlled with medication or laser. It is also the treatment of choice in non-compliant patients, and in infants and children with glaucoma. Filtering microsurgery involves creating a drainage hole with the use of a small surgical tool, to bypass the blockage in the eye's trabecular meshwork (the eye's drainage system). This opening helps increase the flow of fluid out of the eye and thereby reduce the eye pressure.
Some commonly asked questions by glaucoma patients
Q My vision is good, then why do you say I have glaucoma?
A In glaucoma the central vision is not lost till the very late stages. It starts with damage to your peripheral vision and gradually comes to the centre. When the central vision is affected it is too late and nothing can be done to restore vision. In a way, a good vision is misleading as far as severity of glaucoma and extent of damage is concerned.
Q What is the normal pressure for an eye?
A Normal pressure for an eye is one which does not cause any damage to the optic nerve. In most normal people the eye pressure is around 17 to 20 mm of mercury. Some people have higher pressure than this, but that does not cause damage to the nerve for years. However, such patients need careful monitoring so that damage to the nerve is detected at its earliest stage. On the other hand some patients have a much lower eye pressure, say 12 or 14 mm Hg, but this low pressure is not tolerated by the eye and the nerve is damaged. This is a special type of glaucoma and needs more careful monitoring and treatment.
Q How serious is my glaucoma problem?
A It depends upon the amount of optic nerve damage that has already been caused. The damage can be measured by visual field analysis (VFA) and GDx (which measures the thickness of nerve). As the damage is permanent, appropriate measures are taken to prevent or slow down further damage.
Q Is glaucoma preventable?
A Yes, damage due to glaucoma is preventable, not curable. Whatever damage that is already there cannot be restored, however further damage can be arrested or at least slowed down by appropriate treatment. It is a life-long treatment and needs regular followup.
Q Is Glaucoma hereditary?
A Yes, blood related family members of glaucoma patients are likely to develop glaucoma more often than the general population. It is advisable that family members of glaucoma patients should get their eyes review to rule out glaucoma.
Q Can I get back my side vision after treatment?
A Unfortunately the vision loss caused by glaucoma is permanent and cannot be regained.
Q What precaution must one take?
One must remember that glaucoma treatment is life long, and one should use the medicines regularly and should come for follow-up as and when advised.
Persons who are at the risk of developing glaucoma (as listed previously) should undergo regular eye examinations.
Diabetics should ensure good control of blood sugar levels
Avoid smoking
Avoid drinking 2-3 glasses of water at a time.
Q Do I need to come for follow up after laser / surgery?
A Treatment of glaucoma is life-long. Even after laser or surgery one may need additional medication and a lifetime of follow up to monitor the progress of the disease.